A continuous positive airway pressure (CPAP) equipment is often used to treat sleep apnea, which affects millions of Australians. Many individuals believe that since a CPAP mask is too big…
How to choose the best CPAP masks for your sleep position


A continuous positive airway pressure (CPAP) equipment is often used to treat sleep apnea, which affects millions of Australians. Many individuals believe that since a CPAP mask is too big…

If you want to be confident that your CPAP machines and masks are risk-free to use and will continue to help you breathe through the night, regular cleaning is essential.…

How long does sleep apnea last? The answer is no, despite the fact that it is a common question among people with sleep apnea. Despite the fact that there is…

If you're one of the individuals seeking for therapy, you are aware of how much sleep apnea may affect your life. Fortunately, there are several top-notch therapeutic options. Treatment is…

Hormones play a critical role in restful sleep, and getting enough rest is essential for producing those hormones properly. Poor sleep and hormone imbalances can occur even if you practise…

According to published research, both sleep apnea and sleep-disordered breathing greatly raise the risk of stroke. Two patients were studied in this research; both were overweight, elderly ladies who suffered…

Every day, new information emerges shedding light on the crucial function that sleep plays in maintaining overall health. There may be a connection between obstructive sleep apnea (OSA) and the…

Although Obstructive sleep apnea (OSA) has been consistently linked to chronic pain and other health conditions, but do we have any evidence linking OSA to gout? Let’s find out! Understanding…
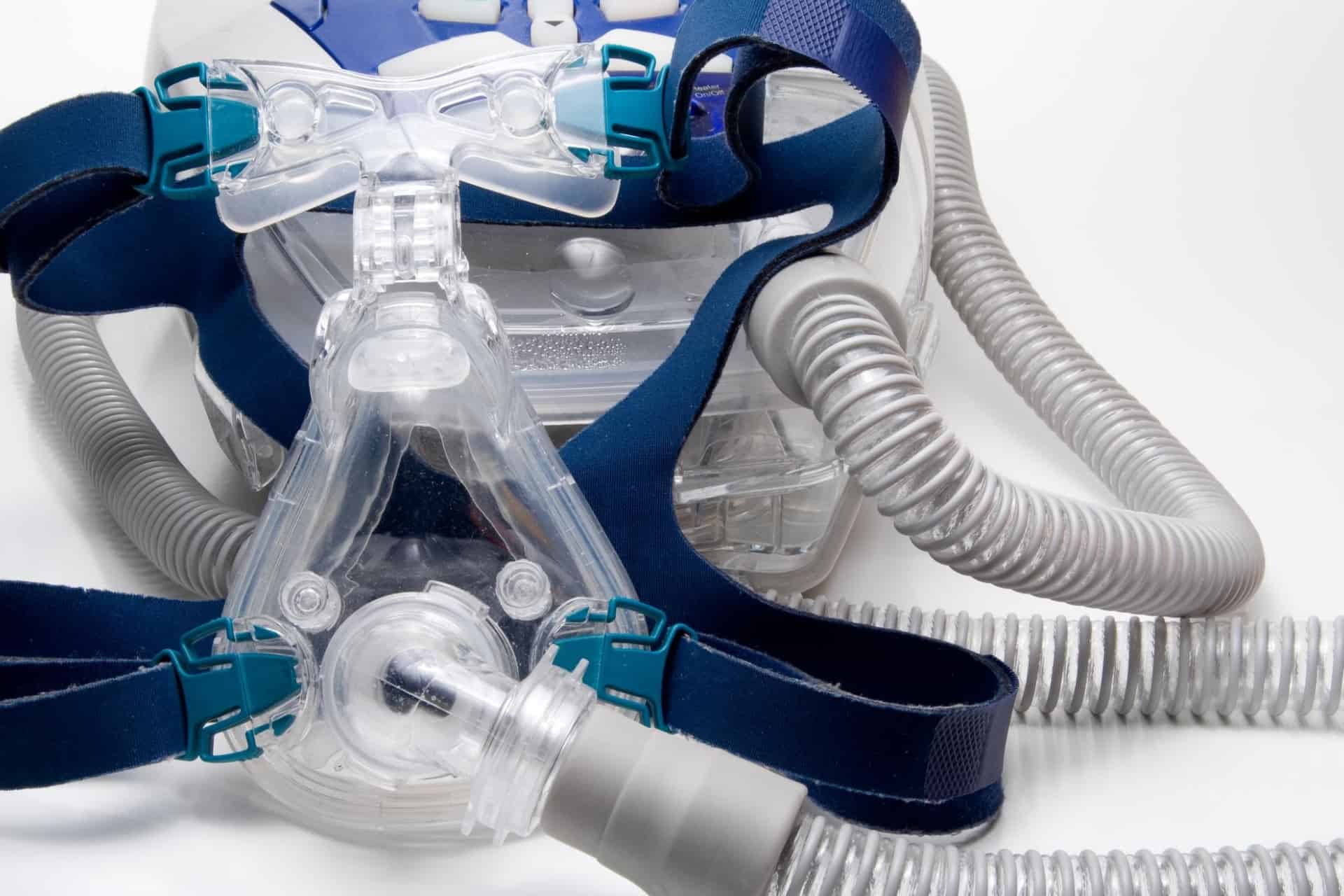
Getting used to sleeping while wearing a CPAP mask and other equipment is a challenge that many people face. We want you to know that you are not alone in…
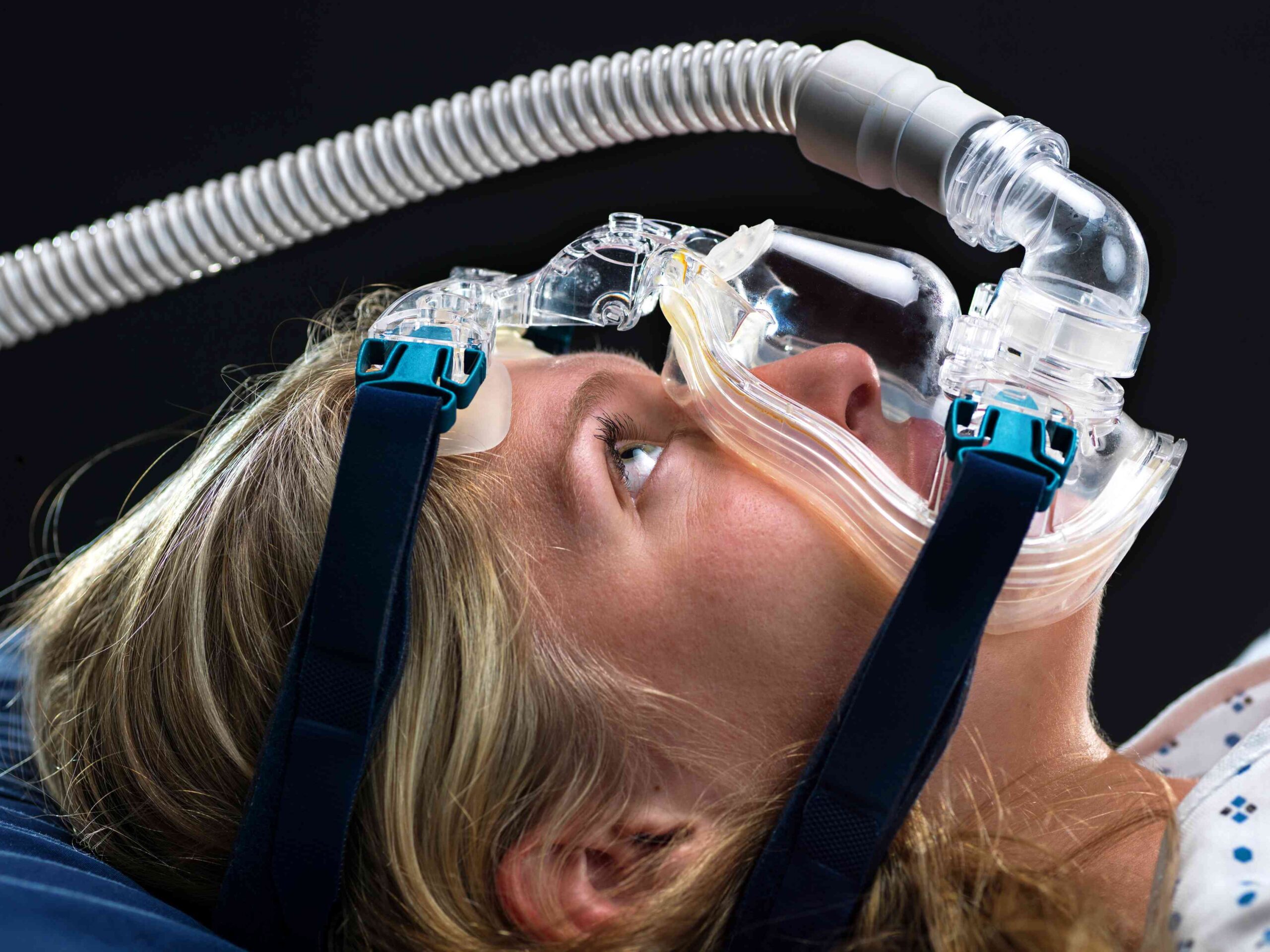
For those who suffer from Sleep Apnea, CPAP therapy can be a challenge to adapt to. You'll need to find a CPAP machine and mask that works for you, and…